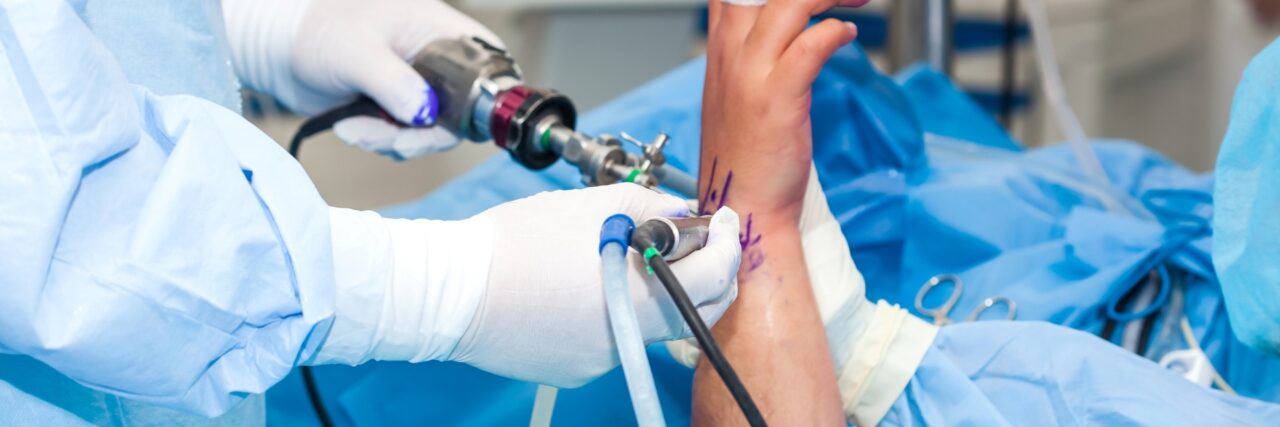
There is no effective means by which the course of Dupuytren’s disease can be altered, so the early, nodular stages are usually a case of observation only. Patients are generally seen by a physician every few months to monitor the extent of the condition. In the later stages, intervention may be required. Needle aponeurotomy is a minimally invasive technique used to treat finger contractures (fingers in a stuck bent position) caused by Dupuytren’s disease.
Minimally Invasive Technique - Dupuytren’s Disease
Needle Aponeurotomy (NA)
Needle aponeurotomy was first developed in France in the 1970’s and popularized by Dr. Eaton in Florida in 2003 as a minimally invasive alternative to open surgical excision. In NA the surgeon uses a needle to cut or divide the contracted palmar cord. This is done through multiple small puncture sites. No open incisions are used.
If performed by properly trained surgeons the procedure is safe.
Procedure
- Your hand will be cleaned and injected with a numbing medication
- A needle will be inserted into the numb area where the tissue is pulling on your fingers creating holes. Multiple puncture sites will be made to rupture and lengthen the tissue.
- Your fingers will then be straightened, separating the tissue and releasing the pull on your fingers.
- Once the procedure is complete, your doctor may inject a steroid medication into your hand to reduce inflammation and swelling.
Goal
Release tight Dupuytrens cords to allow for more extension of the involved digits while avoiding a formation of scar tissue.
Who qualifies?
- Patients with contractures of the middle joint.
Benefits
- The rate of Dupuytrens recurrence has been quoted at 40-65%. The open procedure has an approximate 50% recurrence rate at 5 years while the NA rate is 50% at 3 years.
- Simple technique that avoids unnecessary surgical trauma (minimally invasive)
- Outpatient procedure
- Less than an hour to complete procedure
- Rapid healing
- Procedure can be repeated if deformity occurs
Recovery
- Minimally invasive technique: Immediately the day of surgery the patient can remove the bandages and begin active range of motion. Some numbness may be present for a few hours following surgery. Tingling may also be present in the treated area for about 1-2 days.
- R.I.C.E (link to)
- Avoid full water submersion of hand for 2 days
- A custom nighttime splint is worn for 3 months and night.
- A formal rehabilitation is usually not required.
- Full recovery may take 1-2 weeks.
Complications
- Pain
- Infection
- Scar contraction
- Loss of sensation
- Stiffness
- Damage to nerve or blood vessels
The likelihood of complications may increase depending upon
- The severity of the contracture
- The number of contractures addressed in a single procedure
- The presence of any other medical conditions
Outcomes
- Most patients have improved movement
- About 20% of patients experience some degree of contracture recurrence.
- Some patients may require additional surgery.